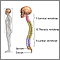
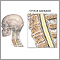
Ankylosing spondylitis
Ankylosing spondylitis is a long-term disease that causes inflammation of the joints between the spinal bones, and the joints between the spine and pelvis. It eventually causes the affected spinal bones to join together.
See also: Arthritis
Causes
The cause of ankylosing spondylitis is unknown, but genes seem to play a role.
The disease most often begins between ages 20 and 40, but may begin before age 10. It affects more males than females. Risk factors include:
- Family history of ankylosing spondylitis
- Male gender
Symptoms
The disease starts with low back pain that comes and goes.
- Pain and stiffness are worse at night, in the morning, or when you are not active. It may wake you from your sleep.
- The pain typically gets better with activity or exercise.
- Back pain may begin in the sacroiliac joints (between the pelvis and the spine). Over time, it may involve all or part of the spine.
You may lose motion or mobility in the lower spine. You may not be able to fully expand your chest because the joints between the ribs are involved.
Fatigue is also a common symptom.
Other, less common symptoms include:
- Eye inflammation or uveitis
- Heel pain
- Hip pain and stiffness
- Joint pain and joint swelling in the shoulders, knees, and ankles
- Loss of appetite
- Slight fever
- Weight loss
Exams and Tests
Tests may include:
- CBC
- ESR
- HLA-B27 antigen
- X-rays of the spine and pelvis
- MRI of the spine
Treatment
Your doctor may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation and pain.
Corticosteroid therapy or medications to suppress the immune system may also be prescribed. Drugs called TNF-inhibitors (etanercept, adalimumab, infliximab), which block an inflammatory protein, have been shown to improve the symptoms of ankylosing spondylitis.
Some health care professionals use drugs that block cell growth (cytotoxic drugs) in people who do not respond well to corticosteroids or who are dependent on high doses of corticosteroids.
Surgery may be done if pain or joint damage is severe.
Exercises can help improve posture and breathing. Lying flat on the back at night can help maintain normal posture.
Outlook (Prognosis)
The course of the disease is unpredictable. Symptoms may come and go at any time. Most people are able to function unless the hips are severely involved.
Possible Complications
Rarely, people may have problems with the aortic heart valve (aortic insufficiency) and heart rhythm problems.
Some patients may have pulmonary fibrosis or restrictive lung disease.
When to Contact a Medical Professional
Call your health care provider if:
- You have symptoms of ankylosing spondylitis
- You have ankylosing spondylitis and develop new symptoms during treatment
Prevention
Prevention is unknown. Awareness of risk factors may allow early detection and treatment.
Alternative Names
Rheumatoid spondylitis; Spondylitis; Spondylarthropathy
References
Goldman L, Ausiello DA. Cecil Medicine. 23rd ed. Philadelphia, Pa: Saunders Elsevier; 2007.
Sidiropoulos PI, Hatemi G, Song IH, et al. Evidence-based recommendations for the management of ankylosing spondylitis: systematic literature search of the 3E Initiative in Rheumatology involving a broad panel of experts and practising rheumatologists. Rheumatology (Oxford). 2008. 47(3):355-61.
Dagfinrud H, Kvien TK, Hagen KB. Physiotherapy interventions for ankylosing spondylitis. Cochrane Database, Syst Rev. 2008. (1):CD002822.
Update Date: 4/21/2012
Reviewed by: Neil J. Gonter, MD, Assistant Professor of Medicine, Columbia University, NY and private practice specializing in Rheumatology at Rheumatology Associates of North Jersey, Teaneck, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.