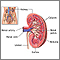
Acute tubular necrosis
Acute tubular necrosis is a kidney disorder involving damage to the tubule cells of the kidneys, which can lead to acute kidney failure.
Causes
Acute tubular necrosis (ATN) is usually caused by lack of oxygen to the kidney tissues (ischemia of the kidneys). It may also occur if the kidney cells are damaged by a poison or harmful substance.
The internal structures of the kidney, particularly the tissues of the kidney tubule, become damaged or destroyed. ATN is one of the most common structural changes that can lead to acute renal failure.
ATN is one of the most common causes of kidney failure in hospitalized patients. Risks for acute tubular necrosis include:
- Blood transfusion reaction
- Injury or trauma that damages the muscles
- Low blood pressure (hypotension) that lasts longer than 30 minutes
- Recent major surgery
- Septic shock due to severe infection
Liver disease and kidney damage caused by diabetes (diabetic nephropathy) may make a person more susceptible to the condition.
ATN can also be caused by:
- Dye (contrast) used for x-ray (radiology) studies
- Medications that are toxic to the kidneys (such as aminoglycoside antibiotics or amphotericin)
Symptoms
- Decreased consciousness
- Decreased urine output or no urine output
- General swelling, fluid retention
- Nausea, vomiting
Note: Other symptoms of acute kidney failure may also be present.
Exams and Tests
The doctor will perform a physical exam. Your doctor may hear abnormal sounds when listening to the heart and lungs with a stethoscope (auscultation). This is due to too much fluid in the body.
Other tests that may be done include:
- BUN and serum creatinine
- Fractional excretion of sodium
- Kidney biopsy
- Urinalysis
- Urine sodium
- Urine specific gravity and osmolarity urine
Treatment
In most people, ATN is reversible. The goal of treatment is to prevent life-threatening complications of acute kidney failure.
Treatment focuses on preventing the excess build-up of fluids and wastes, while allowing the kidneys to heal. Patents should be watched closely for deterioration of kidney function.
Treatment can include:
- Identifying and treating the underlying cause of the problem
- Restricting fluid intake to a volume equal to the volume of urine produced
- Restricting substances normally removed by the kidneys (such as protein, sodium, potassium) to minimize their buildup in the body
- Taking medications to help control potassium levels in the bloodstream
- Medicines taken by mouth or through an IV to help remove fluid from the body
Temporary dialysis can remove excess waste and fluids. This can make you feel better, and may make the kidney failure easier to control. Dialysis may not be necessary for all people, but is often lifesaving, especially if serum potassium is dangerously high.
Dialysis may be needed in the following cases:
- Decreased mental status
- Fluid overload
- Increased potassium levels
- Pericarditis
- To remove toxins that are dangerous to the kidneys
- Total lack of urine production
- Uncontrolled buildup of nitrogen waste products
Outlook (Prognosis)
How long symptoms last can vary. You may make less urin for a few days to 6 weeks or more. This may be followed by a period of high urine output. This occurs because the healed and newly functioning kidneys try to clear the body of fluid and wastes.
One or two days after your urine amount rises, symptoms reduce and test results begin to return to normal.
Possible Complications
- Bleeding from the gastrointestinal tract
- Chronic kidney disease and permanent kidney damage
- High blood pressure
- Increased risk of infection
When to Contact a Medical Professional
Call your health care provider if your urine output decreases or stops, or if you develop other symptoms of acute tubular necrosis.
Prevention
Promptly treating conditions that can lead to decreased blood flow and/or decreased oxygen to the kidneys can reduce the risk of acute tubular necrosis.
Blood transfusions are crossmatched to reduce the risk of incompatibility reactions.
Control conditions such as diabetes, liver disorders, and cardiac disorders to reduce the risk of acute tubular necrosis.
Carefully monitor exposure to medications that can be toxic to the kidney. Have your blood levels of these medications checked regularly. Drink a lot of fluids after having any radiocontrast dyes to allow them to be removed from the body and reduce the risk of kidney damage.
Alternative Names
Necrosis - renal tubular; ATN; Necrosis - acute tubular
References
Clarkson MR, Friedewald JJ, Eustace JA, Rabb H. Acute kidney injury. In: Brenner BM, ed. Brenner: Brenner and Rector's the Kidney. 8th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 29.
Molitoris BA. Acute kidney injury. In: Goldman L, Ausiello D, eds. Cecil Medicine. 23rd ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 121.
Updated: 4/20/2012
Reviewed by: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine; Herbert Y. Lin, MD, PHD, Nephrologist, Massachusetts General Hospital; Associate Professor of Medicine, Harvard Medical School. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.