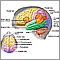
Cluster headache
A cluster headache is one-sided head pain that may involve tearing of the eyes and a stuffy nose. Attacks occur regularly for 1 week to 1 year, separated by long pain-free periods that last at least 1 month, possibly longer.
Other common types of headaches include migraine headache and tension headache .
Causes
Cluster headaches are a fairly common form of chronic, repeated headaches. They are four times more common in men than women. The headaches can occur at any age but are most common in adolescence and middle age. They tend to run in families, passed down through genes.
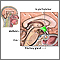
Scientists do not know exactly what causes cluster headaches, but they appear to be related to the body's sudden release of histamine or serotonin. A problem in a small area at the base of the brain called the hypothalamus may be involved.
The following may trigger cluster attacks:
- Alcohol and cigarette smoking
- High altitudes (trekking, air travel)
- Bright light (including sunlight)
- Exertion
- Heat (hot weather, hot baths)
- Foods high in nitrites (such as bacon and preserved meats)
- Certain medications
- Cocaine
Symptoms
A cluster headache begins as a severe, sudden headache. The headache most commonly strikes 2 to 3 hours after you fall asleep. However, the headache may occur while you are awake. The headache tends to occur at the same time of day.
The pain occurs on one side of the head. It may be described as:
- Burning
- Sharp
- Steady
The pain may occur in, behind, and around one eye. It may:
- Involve one side of the face from neck to temples
- Quickly get worse, peaking within 5 to 10 minutes
The strongest pain may last 30 minutes to 2 hours.
The eye and nose on the same side as the head pain may also be affected. Symptoms can include:
- Swelling under or around the eye (may affect both eyes)
- Excessive tearing
- Red eye
- Rhinorrhea (runny nose) or one-sided stuffy nose (same side as the head pain)
- Red, flushed face
Cluster headaches may occur daily for months, alternating with periods without headaches (episodic), or they can recur for a year or more without stopping (chronic).
Exams and Tests
Your health care provider can diagnose this type of headache by performing a physical exam and asking questions about your symptoms and medical history.
If a physical exam is done during an attack, the exam will usually reveal Horner syndrome (one-sided eyelid drooping or a small pupil). These symptoms will not be present at other times. No other nervous system (neurological) changes will be seen.
Tests, such as an MRI of the head, may be needed to rule out other causes of the headaches.
Treatment
Treatment for cluster headaches involves:
- Methods to treat the pain when it happens
- Medicines to prevent the headaches
TREATING CLUSTER HEADACHES WHEN THEY OCCUR
Your doctor may recommend the following treatments for when the headaches occurs:
- Triptans, such as sumatriptan (Imitrex)
- Two to 3 weeks of anti-inflammatory (steroid) medicines such as prednisone -- starting with a high dose, then slowly decreasing it
- Breathing in 100% (pure) oxygen
- Injections of the drug known as dihydroergotamine (DHE), which can stop cluster attacks within 5 minutes (Warning: this drug can be dangerous if taken with sumatriptan)
You may need more than one of these treatments to control headache symptoms. Your doctor may have you try several medications before deciding which works best for you.
Painkillers and narcotics do not usually relieve the pain from cluster headaches. Generally, they take too long to work.
PREVENTING CLUSTER HEADACHES
Avoid smoking, alcohol use, certain foods, and other factors that seem to trigger your cluster headaches. A headache diary can help you identify your headache triggers. When you get a headache, write down the day and time the pain began. The diary should include notes about:
- What you ate and drank in the last 24 hours, how much you slept and when, and what was going on in your life right before the pain started. For example, were you under any unusual stress?
- About how long the headache lasted, and what made it stop.
The headaches may go away on their own, or you may need treatment to prevent them. The following medications may also be used to treat or prevent headache symptoms:
- Blood pressure medicines, such as beta-blockers (propanolol) or calcium channel blockers such as verapamil
- Cyproheptadine
- Drugs used to treat seizures, such as topiramate and valproic acid
- Lithium carbonate
- Medicines used to treat depression, such as amitriptyline
In rare cases, a device that delivers tiny electrial signals to a certain nerve near the brain may be placed. This device is called a neurostimulator. However, it is not yet an established therapy for cluster headaches.
Outlook (Prognosis)
Cluster headaches are not life threatening and usually cause no permanent changes to the brain. However, they are chronic and often painful enough to interfere with work or lifestyle. Rarely, the pain may be so severe that some people may consider harming themselves.
When to Contact a Medical Professional
Call for an appointment with your health care provider if:
- Cluster headaches do not respond to treatment
- Headaches disturb your sleep
- You get headaches whenever you are active
- Headaches occur with other symptoms
Danger symptoms require immediate medical care. Some of these symptoms include:
- Changes in alertness
- Changes in movement or sensation
- Drowsiness
- Nausea or vomiting
- Seizures
- Vision changes
Prevention
If prone to cluster headache, stop smoking. Alcohol use and any foods that are associated with cluster headache may need to be avoided. Medications may prevent cluster headaches in some cases.
Alternative Names
Histamine headache; Headache - histamine; Migrainous neuralgia; Headache - cluster; Horton's headache
References
Francis GJ, Becker WJ, Pringsheim TM. Acute and preventive pharmacologic treatment of cluster headache. Neurology. 2010;75(5):463-473.
Law S, Derry S, Moore RA. Triptans for acute cluster headache. Cochrane Database Syst Rev. 2010;(4)::CD008042.
Silberstein SD, Young WB. Headache and facial pain. In: Goetz CG. Textbook of Clinical Neurology. 3rd ed. St. Louis, Mo: WB Saunders; 2007:chap 53.
Updated: 4/14/2012
Reviewed by: Luc Jasmin, MD, PhD, Department of Neurosurgery at Cedars-Sinai Medical Center, Los Angeles, and Department of Anatomy at UCSF, San Francisco, CA. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Topics
Images
Read More
Patient Instructions
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.