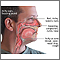
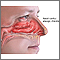
Allergic rhinitis
Allergic rhinitis is a collection of symptoms, mostly in the nose and eyes, which occur when you breathe in something you are allergic to, such as dust, dander, insect venom, or pollen.
This article focuses on allergic rhinitis due to outdoor triggers, such as plant pollen. This type of allergic rhinitis is commonly called hay fever.
For information on other types of allergies, see:
Causes
An allergen is something that triggers an allergy. When a person with allergic rhinitis breathes in an allergen such as pollen or dust, the body releases chemicals, including histamine. This causes allergy symptoms.
Hay fever involves an allergic reaction to pollen. (A similar reaction occurs with allergy to mold, animal dander, dust, and similar allergens that you breathe in.)
The pollens that cause hay fever vary from person to person and from area to area. Tiny, hard to see pollens more often cause hay fever. Examples of plants that cause hay fever include:
- Trees
- Grasses
- Ragweed
The amount of pollen in the air can affect whether hay fever symptoms develop. Hot, dry, windy days are more likely to have increased amounts of pollen in the air. On cool, damp, rainy days most pollen is washed to the ground.
Some disorders may be linked to allergies. These include eczema and asthma.
Allergies are common. Your genes and environment may make you more likely to get allergies.
Whether or not you are likely to develop allergies is often passed down through families. If both your parents have allergies, you are likely to have allergies. The chance is greater if your mother has allergies.
Symptoms
Symptoms that occur shortly after you come into contact with the substance you are allergic to may include:
- Itchy nose, mouth, eyes, throat, skin, or any area
- Problems with smell
- Runny nose
- Sneezing
- Tearing eyes
Symptoms that may develop later include:
- Stuffy nose (nasal congestion)
- Coughing
- Clogged ears and decreased sense of smell
- Sore throat
- Dark circles under the eyes
- Puffiness under the eyes
- Fatigue and irritability
- Headache
- Memory problems and slowed thinking
Exams and Tests
The health care provider will perform a physical exam and ask you questions about your symptoms. Your history of symptoms is important in diagnosing allergic rhinitis. You will be asked whether your symptoms vary by time of day or season, and exposure to pets or other allergens.
Allergy testing may reveal the substances that trigger your symptoms. Skin testing is the most common method of allergy testing. See the article on allergy testing for detailed information.
If your doctor determines you cannot have skin testing, special blood tests may help with the diagnosis. These tests can measure the levels of allergy-related substances, especially one called immunoglobulin E (IgE).
A complete blood count (CBC) test called the eosinophil white blood cell count may also help diagnose allergies.
Treatment
LIFESTYLE AND AVOIDING ALLERGENS
The best treatment is to avoid what causes your allergic symptoms. It may be impossible to completely avoid all your triggers, but you can often take steps to reduce your exposure.
There are many different medications to treat allergic rhinitis. Which one your doctor prescribes depends on the type and severity of your symptoms, your age, and whether you have other medical conditions (such as asthma).
For mild allergic rhinitis, a nasal wash can help remove mucus from the nose. You can buy a saline solution at a drug store or make one at home using one cup of warm water, half a teaspoon of salt, and pinch of baking soda.
Treatments for allergic rhinitis include:
ANTIHISTAMINES
Antihistamines work well for treating allergy symptoms, especially when symptoms do not happen very often or do not last very long.
- Antihistamines taken by mouth can relieve mild to moderate symptoms, but many can cause sleepiness. Some may be bought over the counter, without a prescription. Talk to your doctor before giving these medicines to a child, as they may affect learning.
- Newer antihistamines cause little or no sleepiness. Some are available over the counter. They usually do not interfere with learning. These medications include loratidine (Claritin), fevofenadine (Allegra), and cetirizine (Zyrtec). Other antihistamines are available by prescription.
- Azelastine and astepro (Astelin) and olopatadine (Patanase) are antihistamine nasal sprays that work well for treating allergic rhinitis. You may try these medicines first.
CORTICOSTEROIDS
- Nasal corticosteroid sprays are the most effective treatment for allergic rhinitis.
- They work best when used nonstop, but they can also be helpful when used for shorter periods of time.
- Many brands are available. You will need a prescription from your doctor. They are safe for children and adults.
DECONGESTANTS
- Decongestants may also be helpful for reducing symptoms such as nasal congestion.
- Do not use nasal spray decongestants for more than 3 days.
- Be careful when using over-the-counter saline nasal sprays that contain benzalkonium chloride. These may actually make symptoms worse and cause infection.
OTHER TREATMENTS
- The leukotriene inhibitor Singulair is a prescription medicine approved to help control asthma and to help relieve the symptoms of seasonal allergies.
Specific illnesses that are caused by allergies (such as asthma and eczema) may need other treatments.
ALLERGY SHOTS
Allergy shots (immunotherapy) are sometimes recommended if you cannot avoid the allergen and your symptoms are hard to control. This includes regular injections of the allergen. Each dose is slightly larger than the previous dose. Allergy shots may help your body adjust to the antigen.
For more about treating symptoms in the eyes, see: Allergic conjunctivitis.
Outlook (Prognosis)
Most symptoms of allergic rhinitis can be treated. More severe cases need allergy shots.
Some people (especially children) may outgrow an allergy as the immune system becomes less sensitive to the allergen. However, once a substance causes allergies, it usually continues to affect the person over the long term.
Possible Complications
- Asthma
- Sinusitis
When to Contact a Medical Professional
Call for an appointment with your health care provider if:
- You have severe allergy or hay fever symptoms
- Treatment that once worked for you no longer works
- Your symptoms do not respond to treatment
Prevention
You can sometimes prevent symptoms by avoiding known allergens. During pollen season, people with hay fever should stay indoors where it is air conditioned, if possible.
- Most trees produce pollen in the spring.
- Grasses usually produce pollen during the late spring and summer.
- Ragweed and other late-blooming plants produce pollen during late summer and early autumn.
Alternative Names
Hay fever; Nasal allergies
References
Wallace DV, Dykewicz MS, Bernstein DI, Blessing-Moore J, Cox L, Khan DA, et al. The diagnosis and management of rhinitis: an updated practice parameter. J Allergy Clin Immunol. 2008 Aug:122(2).
Frew AJ. Allergen immunotherapy. J Allergy Clin Immunol. 2010 Feb;125(2 Suppl 2):S306-13.
Sur DK, Scandale S. Treatment of allergic rhinitis. Am Fam Physician. 2010;81:1440-1446.
Updated: 4/1/2012
Reviewed by: Stuart I. Henochowicz, MD, FACP, Associate Clinical Professor of Medicine, Division of Allergy, Immunology, and Rheumatology, Georgetown University Medical School. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Topics
Images
Read More
Patient Instructions
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.