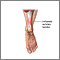
Achilles tendinitis
Achilles tendinitis is when the Achilles tendon becomes swollen, inflamed, and painful at the heel.
The Achilles tendon connects your calf muscles to your heel bone. It is used for walking, running, and jumping.
Causes
There are two large muscles in the calf: the gastrocnemius and the soleus. These muscles create the power needed to push off with the foot or go up on the toes. The large Achilles tendon connects these muscles to the heel.
These are important muscles for walking. This tendon can become inflamed, most commonly as a result of overuse or arthritis. Inflammation can also occur with injury and infection.
Tendinitis due to overuse is most common in younger people. It can occur in walkers, runners, or other athletes. Sports like basketball that involve jumping put a large amount of stress on the Achilles tendon. Repeated jumping can lead to Achilles tendinitis.
Achilles tendinitis may be more likely to occur:
- After a sudden increase in the amount or intensity of an activity
- When the calf muscles are very tight (not stretched out)
Tendinitis from arthritis is more common in middle-aged and elderly people. A bone spur or growth may form in the back of the heel bone. This may irritate the Achilles tendon and cause pain and swelling.
Symptoms
Symptoms include pain in the heel and along the tendon when walking or running. The area may feel painful and stiff in the morning.
The tendon may be painful to touch or move. The skin over the tendon may be swollen and warm. You may have trouble standing up on one toe.
Exams and Tests
The doctor will perform a physical exam. The doctor will look for tenderness along the tendon and pain in the area of the tendon when you stand on your toes.
X-rays can help diagnose arthritis.
An MRI scan may be done if your doctor is thinking about surgery or is worried about the tear in the Achilles tendon.
Treatment
The main treatments for Achilles tendinitis do not involve surgery. It is important to remember that it may take at least 2 to 3 months for the pain to go away.
Try putting ice over the Achilles tendon for 15 to 20 minutes, two to three times per day. Remove the ice if the area gets numb.
Changes in activity may help manage the symptoms:
- Decrease or stop any activity that causes you pain.
- Run or walk on smoother and softer surfaces.
- Switch to biking, swimming, or other activities that put less stress on the Achilles tendon.
Your health care provider or physical therapist can show you stretching exercises for the Achilles tendon.
They may also suggest the following changes in your footwear:
- A brace or boot to keep the heel and tendon still and allow the swelling to go down
- Heel lifts placed in the shoe under the heel
- Shoes that are softer in the areas over and under the heel cushion
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin and ibuprofen can help with pain or swelling. Talk with your health care provider.
If these treatments do not improve symptoms, you may need surgery to remove inflamed tissue and abnormal areas of the tendon. Surgery also can be used to remove the bone spur that is irritating the tendon.
Extracorporeal shock wave therapy (ESWT) may be an alternative to surgery for people who have not responded to other treatments. This treatment uses low-dose sound waves.
Outlook (Prognosis)
Lifestyle changes usually help improve symptoms. However, symptoms may return if you do not limit activities that cause pain, or if you do not maintain the strength and flexibility of the tendon.
Surgery, if needed, has been shown very effective for improving pain.
Possible Complications
Achilles tendinitis may make you more likely to have an Achilles rupture. This condition usually causes a sharp pain, like someone hit you in the back of the heel with a stick. Surgical repair is necessary, but difficult because the tendon is not normal.
When to Contact a Medical Professional
If you have pain in the heel around the Achilles tendon that is worse with activity, contact your health care provider for evaluation and possible treatment for tendinitis.
Prevention
Prevention is very important in this disease. Maintaining strength and flexibility in the muscles of the calf will help reduce the risk of tendinitis. Overusing a weak or tight Achilles tendon makes you more likely to develop tendinitis.
Alternative Names
Tendinitis of the heel
References
Gollwitzer H, Diehl P, von Korff A, Rahlfs VW, Gerdesmeyer L. Extracorporeal shock wave therapy for chronic painful heel syndrome: a prospective, double blind, randomized trial assessing the efficacy of a new electromagnetic shock wave device. J Foot Ankle Surg. 2007;46:348-357.
Baer GS, Keene JS. Tendon injuries of the foot and ankle. In: DeLee JC, Drez D Jr., Miller MD, eds. DeLee and Drez's Orthopaedic Sports Medicine. 3rd ed. Philadelphia, Pa: Saunders Elsevier;2009:section D.
Updated: 4/31/2012
Reviewed by: C. Benjamin Ma, MD, Assistant Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.