Ammonium ion
The ammonium - blood test measures the amount of ammonia in a blood sample.
How the Test is Performed
A blood sample is needed. For information on how this is done, see: Venipuncture
How to Prepare for the Test
Fast for 8 - 12 hours. The health care provider may recommend that you stop taking drugs that may affect your test results.
Drugs that can falsely raise the blood amminia level include alcohol, acetazolamide, narcotics, and valproic acid. A high-protein diet can also raise the blood ammonia level. Talk to your health care provider before this test if you are taking any of these medications.
How the Test Will Feel
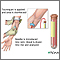
When the needle is inserted to draw blood, you may feel moderate pain, or only a prick or stinging sensation. Afterward, there may be some throbbing.
Why the Test is Performed
This test may be done if you have or are thought to have a condition that may cause a toxic buildup of ammonia. It is most commonly used to diagnose and monitor hepatic encephalopathy, a severe liver disease.
Ammonia (NH3) is produced by cells throughout the body, especially the intestines, liver, and kidneys. Most of the ammonia produced in the body is used by the liver to produce urea. Urea is also a waste product, but it is much less toxic than ammonia.
Ammonia is especially toxic to the brain. It can cause confusion, lethargy, and sometimes coma.
Normal Results
The normal range is 15 - 45 micrograms per deciliter (mcg/dL).
Note: Normal value ranges may vary slightly among different laboratories. Talk to your doctor about the meaning of your specific test results.
The examples above show the common measurements for results for these tests. Some laboratories use different measurements or may test different specimens.
What Abnormal Results Mean
Conditions that can increase ammonia levels include:
- Congestive heart failure
- Gastrointestinal (GI) bleeding - usually in the upper GI tract
- Genetic diseases of the urea cycle
- Hyperthermia (high body temperature)
- Leukemia
- Liver failure
- Muscle exertion
Risks
Veins and arteries vary in size from one patient to another and from one side of the body to the other. Obtaining a blood sample from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight but may include:
- Excessive bleeding
- Fainting or feeling light-headed
- Hematoma (blood accumulating under the skin)
- Infection (a slight risk any time the skin is broken)
Patients with liver disease may have clotting problems. After the venipuncture, pressure should be applied to the puncture site for several minutes to ensure that bleeding has stopped.
Alternative Names
Ammonia level
References
Berk PD, Korenblat KM. Approach to the patient with jaundice or abnormal liver test results. In: Goldman L, Ausiello D, eds. Cecil Medicine. 23rd ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 150.
Nevah MI, Fallon MB. Hepatic encephalopathy, hepatorenal syndrome, hepatopulmonary syndrome, and systemic complications of liver disease. In: Feldman L, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Diseases. 9th ed. Philadelphia, Pa: Saunders Elsevier;2010:chap 92.
Update Date: 2/21/2012
Reviewed by: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.