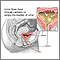
Chronic bilateral obstructive uropathy
Chronic bilateral obstructive uropathy is a long-term blockage of urine flow from both kidneys. It is a slow blockage that gets worse over time.
Bilateral means "both sides."
See also:
Causes
The most common cause of chronic bilateral obstructive uropathy is a condition called bladder outlet obstruction. The kidneys produce urine in the normal manner but the urine cannot leave the bladder. Urine backs up, causing kidney swelling and damage.
When the blockage causes urine to back up into both kidneys, hydronephrosis (swelling of the kidneys) results. High blood pressure and kidney failure can result.
In men, chronic bilateral obstructive uropathy is most often a result a result of enlargement of the prostate, also called benign prostatic hyperplasia (BPH).
Other causes of chronic bilateral obstructive uropathy include:
- Bilateral uretal stones
- Bladder tumors
- Prostate tumors
- Tumors or masses of the uterus or other structures around the bladder neck or urethra
- Retroperitoneal fibrosis or tumor
- Narrowing of the urethra due to a birth defect or scar tissue
- Neurogenic bladder
Chronic bilateral obstructive uropathy occurs in about 1 out of every 1,000 people.
Symptoms
Symptoms depend on the nature of the obstruction and where in the urinary tract the obstruction occurs.
Some of the most common symptoms of chronic obstructive uropathy include:
- Stronger and more frequent urge to urinate
- Difficulty initiating the flow of urine (urinary hesitancy)
- Dribbling of urine, incontinence
- Decreased urine output
- Decrease in the force of the urinary stream
- Increased need to urinate at night
- Burning or stinging with urination
- Feeling of incomplete emptying of the bladder
- Alternating times of increased urine output and decreased urine output
- Fever and chills (if there is also a urinary tract infection)
Additional symptoms that may be associated with this disease:
- Nail problems
- High blood pressure
- Abnormal urine color
Exams and Tests
A physical exam may show swollen or tender kidneys. The bladder may be large and full. A rectal examination may reveal an enlarged prostate. Blood pressure may be high.
Blood tests will be done to check kidney function, electrolyte balance, and blood cell counts. Urine tests may reveal a urinary tract infection.
Other tests that may be done:
- Abdominal ultrasound
- Bladder scan
- CT scan of abdomen and pelvis
- Kidney scan
- Uroflowmetry
Treatment
The goal of treatment is to remove the blockage. You may need to stay in a hospital for a short while.
Treatment may include:
- Antibiotics to treat urinary tract infection
- Catheterization-- the placement of a tube into the body to drain urine (See: Urinary catheters)
- Dialysis if kidney failure occurs
- Laser or heat therapy to shrink the prostate if the problem is due to an enlarged prostate
- Surgery such as transurethral resection of the prostate (TURP)
- Other types of surgery for disorders causing blockage of the urethra or bladder neck
Outlook (Prognosis)
Bilateral obstructive uropathy may be reversible if the blockage is corrected before kidney failure develops.
Chronic kidney failure leads to long-term kidney damage that can be life threatening.
Patients with a chronic blockage are at a higher risk for complications following initial catheter placement. During the first few days following correction of the obstruction, the kidneys may be unable to concentrate urine. As a result, your body removes large amounts of urine that haven't been properly processed. This is called post-obstructive diuresis. It can be a life-threatening condition. Close monitoring is required.
If the obstruction was caused by cancer, the ultimate outcome depends on the disease severity and your response to treatment.
Possible Complications
- Chronic kidney failure
- Complications due to long-term catheter use
- Chronic or recurrent urinary tract infection
- Long-term incontinence or urinary retention
- Formation of uretal or kidney stones
When to Contact a Medical Professional
Call your health care provider if decreased urine output or other symptoms of chronic bilateral obstructive uropathy develop.
Prevention
Routine screening (and treatment) for lower urinary tract disorders may help prevent this condition. A digital rectal exam is used to screen men for prostate problems.
Alternative Names
Obstructive uropathy - bilateral - chronic; Kidney failure - chronic blockage
References
Pais VM Jr, Strandhoy JW, Assimos DG. Pathophysiology of urinary tract obstruction. In: Wein AJ, ed. Campbell-Walsh Urology. 9th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 37.
Hsu THS, Streem SB, Nakada SY. Management of upper urinary tract obstruction. In: Wein AJ, ed. Campbell-Walsh Urology. 9th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 38.
McAninch JW, Santucci RA. Renal and ureteral trauma. In: Wein AJ, ed. Campbell-Walsh Urology. 9th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 39.
Update Date: 3/22/2012
Reviewed by: Linda J. Vorvick, MD, Medical Director, MEDEX Northwest Division of Physician Assistant Studies, University of Washington, School of Medicine; Scott Miller, MD, Urologist in private practice in Atlanta, Georgia. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Topics
Images
Read More
- Acute bilateral obstructive uropathy
- Acute kidney failure
- Benign
- Chronic kidney disease
- Frequent or urgent urination
- Hypertension
- Muscle cramps
- Obstructive uropathy
- Retroperitoneal fibrosis
- Stress incontinence
- Unilateral hydronephrosis
- Urinary incontinence
- Urinary tract infection - adults
- Urinary tract infection - children
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.