Asthma - children
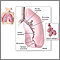
Asthma is a disease of the respiratory system, which causes swelling and narrowing of the airways.
This article discusses asthma in children, also called pediatric asthma. For a more general discussion about the disease, please see asthma.
Causes
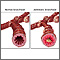
Asthma is caused by swelling and inflammation in the airways. When an asthma attack occurs, the muscles surrounding the airways become tight and the lining of the air passages swells. This reduces the amount of air that can pass by.
Asthma is commonly seen in children. It is a leading cause of hospital stays and school absences. Asthma and allergies often occur together. The allergic response plays a strong role in childhood asthma.
Common asthma triggers include:
- Animals (hair or dander)
- Aspirin and other medications
- Cold air, such as changes in weather (most often cold weather)
- Chemicals in the air or in food
- Dust
- Exercise
- Mold
- Pollen
- Strong emotions
- Tobacco smoke
- Viral infections, such as the common cold
Symptoms
Breathing problems are common. They can include:
- Shortness of breath
- Feeling like you are out of breath
- Gasping for air
- Having trouble breathing out
- Breathing faster than normal
When breathing gets very difficult, the skin of your chest and neck may suck inward.
Other symptoms of asthma in children include:
- Coughing that sometimes wakes the child up at night; it may be the only symptom
- Dark bags under the eyes
- Feeling tired
- Irritability
- Tightness in the chest
- Wheezing, a whistling sound made when breathing, that may be more noticeable when the child breathes out
The type and pattern of your child's asthma symptoms may vary. They may be occur often or only when certain triggers are present. Some children are more likely to have asthma symptoms at night.
Exams and Tests
The doctor will to listen to the child's lungs. Asthma-related sounds may be heard. However, lung sounds are often normal between asthma episodes.
The doctor will have your child breathe into a device called a peak flow meter. Peak flow meters can tell you and your doctor how well the child can blow air out of the lungs. If the airways are narrow and blocked due to asthma, peak flow values drop.
You and your child will learn to measure peak flow at home.
Tests may include:
- Lung function tests
- Chest x-ray
- Allergy testing
- Eosinophil count (a type of white blood cell)
Treatment
You and your child's pediatrician or allergist should work together as a team to create and carry out an asthma action plan.
This plan should outline how to
- Avoid asthma triggers
- Monitor symptoms
- Measure peak flow
- Take medicines
The plan should also tell you when to call the nurse or doctor.
You should also have an emergency plan that outlines what to do when your child's asthma flares up. If your child is in school, make sure teachers, school nurses, physical education teachers, and coaches know about your child's need to take asthma medicine. Find out what you need to do to let your child take his medicine during school hours. (You may need to sign a consent form.) Make sure the school has a copy of your child's asthma action plan. See: Asthma and school
MEDICATIONS
There are two basic kinds of medication for the treatment of asthma:
- Long-term control medications
- Quick relief or "rescue" medications
Long-term control medications are taken every day to prevent asthma symptoms, even when your child does not have symptoms. Some children may need more than one long-term control medication.
Types of long-term control medications include:
- Inhaled steroids (such as Azmacort, Vanceril, AeroBid, Flovent) - these are almost the first choice of treatment
- Leukotriene inhibitors (such as Singulair and Accolate)
- Long-acting bronchodilators (such as Serevent) usually used with inhaled steroids
- Cromolyn sodium (Intal) or nedocromil sodium
- Aminophylline or theophylline (not used as frequently as in the past)
See also: Long-term asthma medicines in children
Quick relief, or rescue, medications are used during an attack. Children who not have symptoms very often (mild asthma) may only need quick relief medication as needed. Examples of quick relief medications include: Proventil, Ventolin, Xopenex, and others.
USING AN INHALER
A number of your child's asthma medicines can be taken using an inhaler.
- Children who use an inhaler should also use a "spacer" device, which helps them to get the medicine into the lung properly.
- If your child uses the inhaler wrong way, less medicine gets into the lungs. Have your health care provider show you how to correctly use an inhaler.
- Younger children can use a nebulizer to take their medicine rather than an inhaler. A nebulizer turns asthma medicine into a mist that you breathe in.
ELIMINATING TRIGGERS
It is important to know what things make your child's asthma worse. These are called asthma "triggers." Avoiding them is the first step toward helping your child feeling better.
If possible, keep pets outdoors, or at least away from the child's bedroom.
No one should smoke in a house or around a child with asthma. Eliminating tobacco smoke from the home is the single most important thing a family can do to help a child with asthma. Smoking outside the house is not enough. Family members and visitors who smoke carry smoke residue in and on their clothes and hair -- this can trigger asthma symptoms.
Keeping humidity levels low and fixing leaks can reduce growth of organisms such as mold. Keep the house clean and keep food in containers and out of bedrooms -- this helps reduce the possibility of cockroaches, which can trigger asthma attacks. Bedding can be covered with "allergy proof" polyurethane-coated casings to reduce exposure to dust mites. Detergents and cleaning agents in the home should be unscented.
All of these efforts can make a significant difference to the child with asthma, even though it may not be obvious right away.
KEEPING AN EYE ON YOUR CHILD'S ASTHMA
A peak flow meter is a simple device that you and your child can use at home to tell you if an attack is coming, maybe before there are any symptoms. Checking "peak flow" is one of the best ways to control asthma. It can help you keep your child's asthma from getting worse. Asthma attacks do NOT usually come on without warning.
Children under age 5 may not be able to use a peak flow meter well enough to make the numbers useful. An adult should always watch carefully for a child's asthma symptoms. It's a good idea to start using peak flow meters before age 5 to get the child used to them.
See also: How to make peak flow measurements a habit
Outlook (Prognosis)
With proper treatment and a team approach to managing asthma, almost all children with asthma can live a normal life. However, poorly controlled asthma may lead to missed school, problems playing sports, missed work for parents, and multiple visits to the doctor's office and emergency room.
Many times, asthma symptoms occur much less often or disappear as the child gets get older. However, if the child’s asthma is not well controlled, it can lead to permanent changes in lung function.
Asthma can rarely be a life-threatening disease. It is important for families to work together with health care professionals to develop a plan to properly care for the child.
Possible Complications
The complications of asthma can be severe. Some include:
- Persistent cough
- Lack of sleep due to nighttime symptoms
- Decreased ability to exercise and take part in other activities
- Missed school
- Missed work for parents
- Emergency room visits and hospital stays
- Trouble breathing that requires breathing assistance (ventilator)
- Permanent changes in the function of the lungs
- Death
When to Contact a Medical Professional
Call your health care provider if you think that a child has new symptoms of asthma. If your child has been diagnosed with asthma, call the doctor:
- After an emergency room visit
- When peak flow numbers have been getting lower
- When symptoms are more frequent and more severe and your child is following the asthma action plan
If your child is having trouble breathing or having an asthma attack, seek medical attention immediately.
Emergency symptoms include:
- Difficulty breathing
- Bluish color to the lips and face
- Severe anxiety due to shortness of breath
- Rapid pulse
- Sweating
- Decreased level of alertness, such as severe drowsiness or confusion
A child who is having a severe asthma may need to stay in the hospital, and may be given oxygen and medicines through a vein (an intravenous line (IV).
Prevention
There is no known method to prevent asthma attacks. The best way to reduce the number of attacks is to avoid triggers (especially cigarette smoke) and follow the asthma plan that you develop with your doctor.
Alternative Names
Pediatric asthma; Asthma - pediatric
References
National Asthma Education and Prevention Program Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma. Rockville, MD. National Heart, Lung, and Blood Institute, US Dept of Health and Human Services; 2007. NIH publications 08-4051.
Castro-Rodriguez JA, Rodrigo GJ. Efficacy of inhaled corticosteroids in infants and preschoolers with recurrent wheezing and asthma: a systematic review with meta-analysis. Pediatrics. 2009 Mar;123(3):e519-25.
Bush A, Saglani S. Management of severe asthma in children. Lancet. 2010 Sep 4;376(9743):814-25.
Brozek JL, Bousquet J, Baena-Cagnani CE, Bonini S, Canonica GW, Casale TB, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J Allergy Clin Immunol. 2010 Sep;126(3):466-76.
Update Date: 5/1/2012
Reviewed by: Neil K. Kaneshiro, MD, MHA, Clinical Assistant Professor of Pediatrics, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Topics
Images
Read More
Patient Instructions
- Asthma and school
- Asthma - control drugs
- Asthma - quick-relief drugs
- Asthma - what to ask your doctor - child
- Exercise-induced asthma
- Exercising and asthma at school
- How to use a nebulizer
- How to use an inhaler - no spacer
- How to use an inhaler - with spacer
- How to use your peak flow meter
- Make peak flow a habit!
- Signs of an asthma attack
- Stay away from asthma triggers
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.