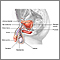
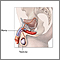
Orchitis
Orchitis is swelling (inflammation) of one or both of the testicles.
Causes
Orchitis may be caused by an infection from many different types of bacteria and viruses.
The most common virus that causes orchitis is mumps. It most often occurs in boys after puberty. Orchitis usually develops 4 - 6 days after the mumps begins. Because of childhood vaccinations, mumps is now rare in the United States.
Orchitis may also occur along with infections of the prostate or epididymis.
Orchitis may be caused by sexually transmitted diseases (STD), such as gonorrhea or chlamydia. The rate of sexually transmitted orchitis or epididymitis is higher in men ages 19 - 35.
Risk factors for sexually transmitted orchitis include:
- High-risk sexual behaviors
- Multiple sexual partners
- Personal history of gonorrhea or another STD
- Sexual partner with a diagnosed STD
Risk factors for orchitis not due to an STD include:
- Being older than age 45
- Long-term use of a Foley catheter
- Not being vaccinated against the mumps
- Problems of the urinary tract that occurred at birth (congenital)
- Regular urinary tract infections
- Surgery of the urinary tract (genitourinary surgery)
Symptoms
- Blood in the semen
- Discharge from penis
- Fever
- Groin pain
- Pain with intercourse or ejaculation
- Pain with urination (dysuria)
- Scrotal swelling
- Tender, swollen groin area on affected side
- Tender, swollen, heavy feeling in the testicle
- Testicle pain that is made worse by a bowel movement or straining
Exams and Tests
A physical examination may show:
- Enlarged or tender prostate gland
- Tender and enlarged lymph nodes in the groin (inguinal) area on the affected side
- Tender and enlarged testicle on the affected side
Tests may include:
- Complete blood count (CBC)
- Testicular ultrasound
- Tests to screen for chlamydia and gonorrhea (urethral smear)
- Urinalysis
- Urine culture (clean catch) -- may need several samples, including initial stream, midstream, and after prostate massage
Treatment
Treatments may include:
- Antibiotics -- if the infection is caused by bacteria (in the case of gonorrhea or chlamydia, sexual partners must also be treated)
- Anti-inflammatory medications
- Pain medications
- Bed rest with the scrotum elevated and ice packs applied to the area
Outlook (Prognosis)
Getting the right diagnosis and treatment for orchitis caused by bacteria can usually preserve the normal testicle function.
If the testicle does not completely return to normal after treatment, further testing to rule out testicular cancer should be done.
Mumps orchitis cannot be treated, and the outcome can vary. Men who have had mumps orchitis can become sterile.
Possible Complications
Some boys who get orchitis caused by mumps will have shrinking of the testicles (testicular atrophy).
Orchitis may also cause infertility.
Other potential complications include:
- Chronic epididymitis
- Death of testicle tissue (testicular infarction)
- Fistula on the skin of the scrotum (cutaneous scrotal fistula)
- Scrotal abscess
Acute pain in the scrotum or testicles can be caused by twisting of the testicular blood vessels (torsion), which is a surgical emergency. If you have sudden pain in the scrotum or testicles, get immediate medical attention.
When to Contact a Medical Professional
All testicle abnormalities should be medically evaluated. Call the local emergency number (such as 911) or go to the nearest emergency room if you experience sudden pain in the testicle.
Prevention
Getting vaccinated against mumps will prevent mumps-associated orchitis. Safer sex behaviors, such as having only one partner at a time (monogamy) and condom use, will decrease the chance of developing orchitis as a result of a sexually transmitted disease.
Alternative Names
Epididymo-orchitis; Testis infection
References
Krieger JN. Prostatitis, epididymitis, and orchitis. In: Mandell GL, Bennett JE, Dolin R, eds. Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, Pa: Elsevier Churchill Livingstone;2009:chap 109.
MacDonald NE. Epididymitis, orchitis, and prostatitis. in: Long SS, ed. Principles and Practice of Pediatric Infectious Diseases. 3rd ed. Philadelphia, Pa: Elsevier Churchill Livingstone;2008:chap 57.
Updated: 4/3/2012
Reviewed by: Linda J. Vorvick, MD, Medical Director, MEDEX Northwest Division of Physician Assistant Studies, University of Washington School of Medicine; and Scott Miller, MD, Urologist in private practice in Atlanta, Georgia. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.