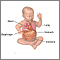
Diaphragmatic hernia repair - congenital
Diaphragmatic hernia repair is surgery to correct a birth defect called a diaphragmatic hernia. The diaphragm is a large dome-shaped muscle that separates the chest cavity (where your heart and lungs are) from the belly area.
The diaphragm is a very important muscle for breathing. Diaphragmatic hernias in babies are vary rare, and are almost always found soon after birth.
A diaphragmatic hernia is an opening or tear in the diaphragm. In a child born with a diaphragmatic hernia, the organs from the belly (stomach, spleen, liver, and intestines) may go up into the chest cavity where the lungs are. These abdominal organs take up the space and prevent the lung from growing normally. As a result, the lung stays too small for children to breathe on their own when they are born.
Description
Before surgery, some infants may need a breathing device to improve their oxygen levels.
Surgery is done while your child is under general anesthesia (asleep and not able to feel pain). The surgeon makes a surgical cut in the abdomen under the upper ribs to be able to reach the organs of the abdomen. Then the surgeon gently pulls these organs down into place through the opening in the diaphragm and into the abdominal cavity.
The surgeon repairs the hole in the diaphragm. If the hole is small, it may be repaired with stitches, but in most cases a piece of plastic patch is used to cover the hole in the diaphragm.
After surgery, a tube from the chest will stay in place for a few days to allow air, blood, and fluid to drain. The increased room in the chest will now allow the lungs room to expand.
Why the Procedure is Performed
A diaphragmatic hernia can be life threatening. Surgery to repair it must be done in the first few days or weeks of a child’s life.
Risks
Risks for this surgery include:
- Breathing problems, which may be severe
- Bleeding
- Infection
- Reactions to medicines
Other possible complications of this surgery include:
- Collapsed lung
- Lung problems that do not go away
- Respiratory failure
Before the Procedure
Infants with a diaphragmatic hernia are transferred to a neonatal intensive care unit (NICU). It may take days or weeks for your child's health to be stable enough for surgery.
- In the NICU, your child will probably need help breathing with a breathing machine (mechanical ventilator) before the surgery. This is because the lungs are smaller than normal.
- If your child is very sick, their doctor may use a heart-lung bypass machine (ECMO) to help the child get well enough for surgery. This machine does the work of the heart and lungs for your child.
- Before surgery, the hospital staff will take x-rays and perform regular blood tests to see how well your child's lungs are working. Your child will also have a light sensor (called a pulse oximeter) taped to the skin to monitor the oxygen level in the blood.
- Your child may also be on medicines to control the blood pressure and keep him or her comfortable.
Your child will also have a tube going from the mouth to the stomach to keep air out of the stomach. There will also be a catheter (tube) placed in an artery (to monitor the blood pressure) and a vein (to deliver nutrients and medicines).
After the Procedure
Your child will stay in the hospital for several weeks after the surgery. Your child will be on a breathing machine after the surgery. Once the baby is taken off the breathing machine, he or she may still need oxygen and some medicine for a while.
Feedings will start after your child's bowels start working. Feedings are usually done through a feeding tube from the mouth into the stomach or small intestines until your child can take all the food he or she needs by mouth.
Most infants with diaphragmatic hernias have reflux when they eat. This means the food or acid in their stomach moves up into their esophagus (the tube that leads from the throat to the stomach). This can be uncomfortable for your child. It also leads to frequent spitting up, vomiting, and pneumonia, which makes feedings more difficult once your child is taking food by mouth.
The nurses and feeding specialists will teach you ways to hold and feed your baby to prevent reflux. Some children need to be on a feeding tube for a long time to get enough food to grow.
Outlook (Prognosis)
The outcome of this surgery depends on how well your baby's lungs have developed. Some babies have other medical problems, including problems with the brain, muscles, and joints, that may slow recovery.
Usually the outlook is good for infants who have well-developed lung tissue. Most babies with a diaphragmatic hernia from birth (congenital) are very ill and will stay in the hospital for a long time. With advances in medicine, the outlook for these infants is gradually improving.
All children who have had diaphragmatic hernia repairs will need to be watched closely to make sure the hole in their diaphragm does not open up again as they grow.
Children who had a large opening or defect in the diaphragm, or who had more problems with their lungs after birth, may have lung disease after they leave the hospital. They may need oxygen, medicines, and a feeding tube for months or years.
Some children will have problems crawling, walking, talking, and eating. They will need to see physical or occupational therapists to help them develop muscles and strength.
References
Maheshwari A, Carlo WA. Diaphragmatic hernia. In: Kliegman RM, Behrman RE, Jenson HB, Stanton, BF, eds. Nelson Textbook of Pediatrics. 19th ed. Philadelphia, Pa: Saunders Elsevier; 2011:chap 95.8.
Ehrlich PF, Coran AG. Diaphragmatic hernia. In: Kliegman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. 18th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 101.
Puri P, Nakazawa N. Congenital diaphragmatic hernia. In: Puri P, Hollworth M, eds. Pediatric surgery: diagnosis and management. Springer; 2009:chap 31.
Updated: 4/21/2012
Reviewed by: Shabir Bhimji MD, PhD, Specializing in General Surgery, Cardiothoracic and Vascular Surgery, Midland, TX. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.