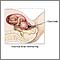
Fetal heart monitoring
Fetal heart monitoring lets the health care provider monitor the baby's heartbeat in the uterus, including during labor. The procedure can be done with monitors outside the body (external monitoring) or in the uterus (internal monitoring).
How the Test is Performed
EXTERNAL FETAL MONITORING
By definition, external fetal monitoring is done through the skin and is not meant to be invasive. You will sit with knees and back partially elevated with a cushion under the right hip, which moves your uterus to the left. You can also sit in other comfortable positions, as long as your uterus is shifted to the left or, for brief periods, to the right.
Sensitive electrodes (connected to monitors) are placed on your abdomen over conducting jelly. The electrodes can sense the fetal heart rate (FHR) and the presence and duration of uterine contractions. Usually, the results of this test are continuous and are printed out, or they appear on a computer screen. External monitors, however, cannot tell how strong contractions are.
This allows your health care provider to check if your baby’s pattern is one seen in healthy babies, and how well the baby is tolerating the contractions. The decision to move to internal fetal monitoring is based on the information first obtained by external fetal monitoring.
NONSTRESS TEST
The nonstress test is another way of externally monitoring your baby. The nonstress test can be done as early as the 27th week of pregnancy, and it measures the FHR accelerations with normal movement. For this test, you will sit with knees and back partially elevated with a cushion under the right hip, which moves your uterus to the left.
The same monitors described above are placed on your abdomen to measure the FHR pattern and whether the uterus is contracting. If there is no fetal heart rate reactivity after 30 - 40 minutes (indicated by a rise in the baby’s heart beat above its baseline with fetal movement), you will be given something to drink or a small meal which may stimulate fetal activity. Other interventions that might encourage fetal movement include the use of fetal acoustic stimulation (sending sounds to the fetus) and gently placing your hands on your abdomen and moving the fetus.
CONTRACTION STRESS TEST
The contraction stress test is a final method of externally monitoring your baby. This test measures the ability of the placenta to provide enough oxygen to the fetus while under pressure (contractions).
For this test, you will sit with knees and back partially elevated with a cushion under the right hip, which moves your uterus to the left. The same monitors described above are placed on your abdomen to measure uterine contractions and FHR. If contractions are not occurring spontaneously, either a medication (called oxytocin) will be given intravenously, or nipple stimulation will be used to induce contractions.
If oxytocin is administered, it is called the oxytocin challenge test. Oxytocin is administered through an IV until 3 uterine contractions are observed, lasting 40 - 60 seconds, over a 10-minute period.
Another test is called the nipple stimulation contractions stress test. Every effort will be taken to ensure your privacy, but the nurse will be with you through the entire procedure.
In this test, you will rub the palm of your hand across one nipple through your garments for 2 - 3 minutes. After a 5-minute rest, the nipple stimulation should continue until 40 minutes have elapsed, or 3 contractions have occurred, lasting more than 40 seconds, within a 10-minute period. If a uterine contraction starts, you should stop the nipple stimulation.
INTERNAL FETAL MONITORING
Internal fetal monitoring involves placing a electrode directly on the fetal scalp through the cervix. Your health care provider may use this method of monitoring your baby if external monitoring is not working well, or the information is suspicious.
A vaginal examination will be performed, and the electrode will be introduced with its plastic sheath into the vaginal canal. This plastic guide is moved through the cervix and placed on the fetus' scalp, then removed. The electrode's wire is strapped to your thigh, and attached to the monitor.
How to Prepare for the Test
Your health care provider will explain the procedure and its risks. You will be asked to wear a hospital gown and sign a consent form prior to the procedure.
How the Test Will Feel
External fetal monitoring:
- Sitting in place for extended periods of time can become uncomfortable for some women. If this is the case, your health care provider can help reposition you to a more comfortable position.
- The ultrasound jelly may feel cold.
Internal fetal monitoring:
- Some women report feeling mild discomfort as the electrode is inserted through the cervix.
Why the Test is Performed
Both types of tests are performed to evaluate fetal heart rate and variability between beats, especially in relation to uterine contractions. The tests also indicate the frequency and strength of uterine contractions.
This information is invaluable in determining how well your baby is tolerating the birth process, and if there needs to be emergency intervention.
Normal Results
Normal values show a fetal heart rate between 120 and 160 beats per minute and are a sign that the developing baby is not in distress. The heart beat may vary 5 - 25 beats per minute from the baseline (normal) fetal heart rate.
A rise above baseline with fetal movement is a reassuring sign.
The fetal heart rate may drop slightly during a contraction. This is normal as long as the fetal heart rate recovers quickly once the contraction has stopped.
What Abnormal Results Mean
Fetal heart monitoring tests can detect the following abnormal situations or conditions during pregnancy:
- Reduced blood flow to the developing baby (cord compression)
- Block of electrical signals within the heart muscle, causing an altered heart beat (fetal heart block)
- Incorrect positioning of the baby (fetal malposition)
- Too little oxygen supply to the developing baby (potential fetal hypoxia)
- Infection (monitoring cannot diagnose an infection, but can suggest the presence of an infection)
- Too little oxygen exchange between the uterus and the placenta (uteroplacental insufficiency)
- Fetal distress
- Abruptio placenta
- Severe anemia in the developing baby
Risks
External fetal monitoring:
- There are no risks associated with external monitoring. Some people believe the test, however, may lead to early delivery, unnecessary cesarean section, and other more invasive forms of delivery. Talk to your health care provider about the use of external monitoring.
Internal fetal monitoring:
- Infection
- Fetal scalp bruising
Alternative Names
Nonstress test; Contraction stress test; Scalp monitoring
References
Druzin ML, Smith JF Jr, Gabbe SG, Reed KL. Antepartum fetal evaluation. In: Gabbe SG, Niebyl JR, Simpson JL, eds. Obstetrics: Normal and Problem Pregnancies. 5th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2007:chap 11.
Garite TJ. Intrapartum fetal evaluation. In: Gabbe SG, Niebyl JR, Simpson JL, eds. Obstetrics: Normal and Problem Pregnancies. 5th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2007:chap 15.
Farley D, Dudley DJ. Fetal Assessment During Pregnancy. Pediatric Clinics of North America. June 2009;56(3).
Update Date: 2/22/2012
Reviewed by: Linda J. Vorvick, MD, Medical Director, MEDEX Northwest Division of Physician Assistant Studies, University of Washington, School of Medicine; Susan Storck, MD, FACOG, Chief, Eastside Department of Obstetrics and Gynecology, Group Health Cooperative of Puget Sound, Redmond, Washington; Clinical Teaching Faculty, Department of Obstetrics and Gynecology, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.