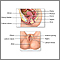
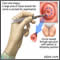
Cold knife cone biopsy
A cold knife cone biopsy (conization) is a procedure to get a sample of abnormal tissue from the cervix for further examination.
See also: Colposcopy-directed biopsy
How the Test is Performed
This is a surgical procedure. It is done in the hospital while you are either sedated through an IV or under general anesthesia.
You will lie on a table and place your feet in stirrups to position your pelvis for examination. The doctor will insert an instrument (speculum) into your vagina to open the vaginal walls and examine the cervix.
A small cone-shaped sample of tissue is removed from the cervix and examined under a microscope for any signs of cancer. This biopsy may also be the treatment if the doctor removes all of the diseased tissue.
How to Prepare for the Test
As with any procedure that is done under anesthesia, you will probably need to fast for 6 - 8 hours. You must sign an informed consent form. The procedure is done on the same day (outpatient) and a hospital stay is usually not needed.
How the Test Will Feel
After the procedure, you may have some cramping or discomfort for a week or so. For about 4 - 6 weeks avoid:
- Douching (you should never do this in any case)
- Sexual intercourse
- Using tampons
For 2 - 3 weeks after the procedure, you may have discharge that is:
- Bloody
- Heavy
- Yellow-colored
Why the Test is Performed
Before colposcopy was commonly used, cold knife cone biopsy was the standard next step to diagnose the cause of worrisome Pap smear results. Now, colposcopy is almost always the first step.
A cold knife biopsy may be done if a cervical biopsy using colposcopy cannot find the cause of an abnormal Pap smear.
Conization may also be used to treat moderate to severe biopsy results (CIN II or III). Very early stage cervical cancer (stage 0 or IA1) may be treated with conization. Abnormal cells from the cervical canal, including adenocarcinoma in situ, may be diagnosed, and sometimes treated with cone biopsy.
Normal Results
There are no precancerous or cancerous cells in the cervix.
What Abnormal Results Mean
Most often, abnormal results mean that there is an area of precancerous or cancerous cells.
Risks
- Bleeding
- Incompetent cervix (which may lead to premature delivery)
- Infection
- Scarring of the cervix (which may cause painful menstrual periods, make it more difficult for doctors to read an abnormal Pap smear, increase the chance for premature delivery, and make it harder to become pregnant)
Alternative Names
Cone biopsy; Biopsy - cone; Cervical conization
References
Noller KL. Intraepithelial neoplasia of the lower genital tract (cervix, vulva): Etiology, screening, diagnostic techniques, management. In: Katz VL, Lentz GM, Lobo RA, Gershenson DM, eds. Comprehensive Gynecology. 5th ed. Philadelphia, Pa: Mosby Elsevier; 2007:chap 28.
American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 99: Management of abnormal cervical cytology and histology. Obstet Gynecol. 2008;112:1419-1444.
Update Date: 2/21/2012
Reviewed by: Susan Storck, MD, FACOG, Chief, Eastside Department of Obstetrics and Gynecology, Group Health Cooperative of Puget Sound, Redmond, Washington; Clinical Teaching Faculty, Department of Obstetrics and Gynecology, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
Notice: The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.