How are your local NHS services coping this winter?
Simultaneous big waves of Covid and flu – the ‘twindemic’ experts warned of as people returned to ‘normal’ pre-pandemic mixing – cost the NHS this winter, say NHS bosses.
NHS England chief strategy officer Chris Hopson said hospital pressures in England peaked on 29 December.
The workload involved gave hospitals a “significant problem” at the turn of the year, he said.
It was at this point that record-long waits at A&E were seen.
Since then the pressures have begun to ease a little.
Speaking to MPs on the House of Commons’ health committee, Mr Hopson said: “The issue was always going to be this winter was the degree to which we saw prevalence of both Covid and flu and the degree to which they combined.
“Now we’re obviously not through winter yet but the really important point – that I don’t think has come out enough – is both Covid and flu peaked so far on 29 December.”
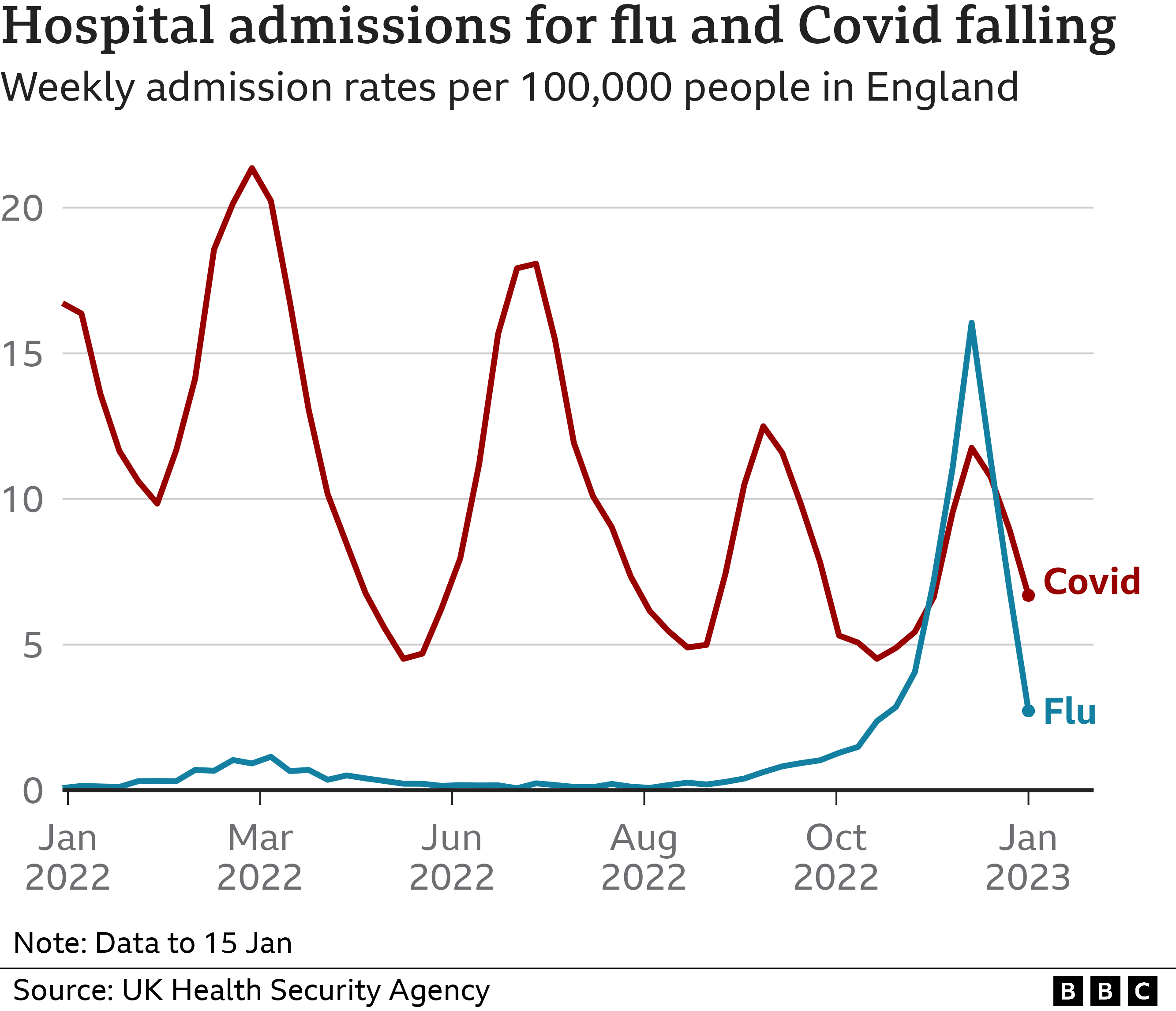
He suggested that when NHS bosses were planning for winter that was very much the worst scenario.
At the turn of the year one in eight beds were occupied by patients with either Covid or flu.
And Mr Hopson added this combined with the 12,000 beds occupied by patients medically fit to leave but unable to be discharged because of the lack of support in the community meant more than a quarter of beds were lost.
“It gives a significant problem in terms of patient flow, which then means you get the back up right the way through the system.”
During the last week of 2022 that more than 40% of ambulances arriving at A&Es faced delays handing over patients to hospital staff.
This contributed to record long waiting times for ambulances to get out to new cases, while inside A&E more than a third of patients were waiting over four hours.
Earlier in the session Adrian Boyle, of the Royal College of Emergency Medicine, described it as the NHS’ worst-ever December.
But he said there was a “complex” range of factors that contributed to the pressures, including staffing shortages and a lack of beds after significant cuts to bed numbers over the years, which has left the NHS with one of the lowest number per head of population in western Europe.
“There is no magic fix,” he added.
About the data
Data for England is shown by NHS trust, where the trust includes at least one hospital with a Type 1 AE department. Type 1 means a consultant-led 24 hour AE service with full resuscitation facilities. Data for Wales and Scotland is shown by Health Board and in Northern Ireland by Health and Social Care Trust.
When you enter a postcode for a location in England you will be shown a list of NHS trusts in your area. They will not necessarily be in order of your closest hospital as some trusts have more than one hospital. Data for Wales and Scotland are shown by NHS board and by Health and Social Care trust in Northern Ireland.
Comparative data is shown for a previous year where available. However, where trusts have merged there is no like-for-like comparison to show. Earlier data is not available for all measures, so comparisons between years are not always possible.
AE attendances include all emergency departments in that trust or health board, not just major AE departments, for example, those who attend minor injury units.
Each nation has different target times for some of the measures shown, therefore comparisons between them may not be possible.

